Overview of Low Back Pain
A Patient's Guide to Low Back Pain (overview)
Introduction
The spine is one of the most important parts of your body. Without it, you could not keep yourself upright or even stand up. It gives your body structure and support. It allows you to move about freely and to bend with flexibility. The spine is also designed to protect your spinal cord. The spinal cord is a column of nerves that connects your brain with the rest of your body, allowing you to control your movements. Without a spinal cord, you could not move any part of your body, and your organs could not function. This is why keeping your spine healthy is vital if you want to live an active life.
Anatomy
The parts of your spine and how they work
What exactly is the spine? Your spine is made up of 24 small bones (vertebrae) that are stacked on top of each other to create the spinal column. Between each vertebra is a soft, gel-like cushion called a disc that helps absorb pressure and keeps the bones from rubbing against each other. Each vertebra is held to the others by groups of ligaments. Ligaments connect bones to bones; tendons connect muscles to bones. There are also tendons that fasten muscles to the vertebrae. The spinal column also has real joints (just like the knee or elbow or any other joints) called facet joints. The facet joints link the vertebrae together and give them the flexibility to move against each other.
Each vertebra has a hole in the center, so when they stack on top of each other they form a hollow tube that holds and protects the entire spinal cord and its nerve roots. The spinal cord itself is a large collection of nerve tissue that carries messages from your brain to the rest of your body. In order for your body to function, you need your nerves. The spine branches off into thirty-one pairs of nerve roots. These roots exit the spine on both sides through spaces (neural foramina) between each vertebra.
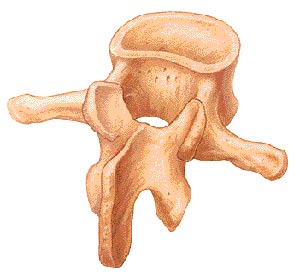
The spine itself has three main segments: the cervical spine, the thoracic spine, and the lumbar spine. The cervical is the upper part of the spine, made up of seven vertebrae (bones). The thoracic is the center portion of the spine, consisting of 12 vertebrae. The lower portion of the spine is called the lumbar spine. It is usually made up of five vertebrae, however, some people may have six lumbar vertebrae. Having six vertebrae does not seem to cause a problem. Below the lumbar spine is the sacrum. The sacrum is actually a group of specialized vertebrae that connects the spine to the pelvis. During development (those nine months before birth), these vertebrae grow together (or fuse) creating one large "specialized" vertebral bone that forms the base of your spine and center of your pelvis. The nerves that leave the spine in the sacral region control the bowel and bladder functions and give sensation (feeling) to the crotch area.
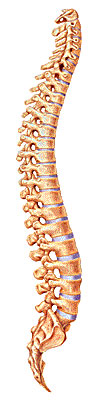
The normal spine has an "S"-like curve when looking at it from the side. This allows for an even distribution of weight. The "S" curve helps a healthy spine withstand all kinds of stress. The cervical spine curves slightly inward, the thoracic curves outward, and the lumbar curves inward. Even though the lower portion of your spine holds most of the body's weight, each segment relies upon the strength of the others to function properly.
Now, let' s look at the specific parts that make up your spine:
Vertebrae
The individual bones of the spine are the vertebrae. These are the building blocks of the spinal column. The vertebrae protect and support the spinal cord. They also bear the majority of the weight put upon your spine. The body of each vertebra is the large, round portion of bone. The body of each vertebra is attached to a bony ring. When the vertebrae are stacked one on top of the other, this ring creates a hollow tube where the spinal cord passes through.
The bony ring attached to the vertebral body consists of several parts. First, the laminae extend from the body to cover the spinal canal, which is the hole in the center of the vertebrae. Second, the spinous process is the bony portion opposite the body of the vertebra. You feel this part if you run your hand down a person's back. Then there are two transverse processes (little bony bumps), where the back muscles attach to the vertebrae. Finally, the pedicle is a bony projection that connects to both sides of the lamina.
The vertebra, like all bones, has an outer shell called cortical bone that is hard and strong. The inside is made of a soft, spongy type of bone called cancellous bone.
Intervertebral Disc
The intervertebral discs are flat, round "cushions" that act as shock absorbers between each vertebra in your spine. There is one disc between each vertebra. Each disc has a strong outer ring of fibers called the annulus, and a soft, jelly-like center called the nucleus pulposus.
The annulus is the disc's outer layer and the strongest area of the disc. It also helps keep the disc's center intact. The annulus is actually a strong ligament that connects each vertebra together.
The mushy nucleus of the disc serves as the main shock absorber. The nucleus is made up of tissue that is very moist because it has high water content. The water content helps the disc act like a shock absorber - somewhat like a waterbed mattress.
Facet Joint
The facets are the "bony knobs" that meet between each vertebra to form the facet joints that join your vertebrae together. There are two facet joints between each pair of vertebra, one on each side. They extend and overlap each other to form a joint between the neighboring vertebra facet joints. Without the facet joints, you would not have flexibility in your spine, and you could only move in very straight and stiff motions.
The facet joints are what are known as synovial joints. A synovial joint, such as the knee or elbow, is a structure that allows movement between two bones. In a synovial joint, the ends of the bones are covered with a material called articular cartilage. This material is a slick, spongy material that allows the bones to glide against one another without much friction.
Surrounding the facet joint is a watertight sack made of soft tissue and ligaments. This sack creates what is called the "joint capsule". The ligaments are soft tissue structures that hold the two sides of the facet joint together. The ligaments around the facet joint combine with the synovium to form the joint capsule that is filled with fluid (synovial fluid). This fluid lubricates the joint to decrease the friction, just like oil lubricates the moving parts of a machine.
Neural Foramen
The neural foramen is the opening between every two vertebrae where the nerve roots exit the spine. The nerve roots travel through the foramen to reach the rest of your body. There are two neural foramina between each pair of vertebrae - one on each side. Without the foramen, nerve signals could not travel to and from the brain to the rest of your body. Without nerve signals, your body would not be able to function.
Spinal Cord and Nerve Roots
The spinal cord is a column of millions of nerve fibers that run through your spinal canal. It extends from the brain to the area between the end of your first lumbar vertebra and top of your second lumbar vertebra. At the second lumbar vertebra, the spinal cord divides into several different groups of fibers that form the nerves that will go to the lower half of the body. For a small distance, the nerves actually travel through the spinal canal before exiting out the neural foramen. This collection of nerves is called the cauda equina while it is still inside the spinal canal.
A protective membrane called the dura mater covers the spinal cord. The dura mater forms a watertight sack around the spinal cord and the spinal nerves. Inside this sack, the spinal cord is surrounded by spinal fluid.
The nerve fibers in your spinal cord branch off to form pairs of nerve roots that travel through the small openings (foramina) between your vertebrae. The nerves in each area of the spinal cord connect to specific parts of your body. This is why damage to the spinal cord can cause paralysis in certain areas and not others -- it depends on which spinal nerves are affected. The nerves of the cervical spine go to the upper chest and arms. The nerves in your thoracic spine go to your chest and abdomen. The nerves of the lumbar spine then reach to your legs, bowel, and bladder. These nerves coordinate and control all the body's organs and parts, and let you control your muscles.
The nerves also carry electrical signals back to the brain that allow you to feel sensations. If your body is being hurt in some way, your nerves signal the brain that you have been hurt. Damage to the nerves themselves can cause pain, tingling, or numbness in the area where the nerve travels.
Paraspinal Muscles
The paraspinal muscles refer to the muscles next to the spine. They support the spine and are the motor for movement of the spine. Your joints allow flexibility and your muscles allow mobility. There are many small muscles in the back - each controlling some part of the total movement between all the vertebrae and the rest of the skeleton. These muscles can be injured directly, such as when you have a pulled muscle or muscle strain of the back muscles. The muscles can also cause problems indirectly, such as when the muscles are in spasm after injury to other parts of the spine.
When you experience a muscle spasm, it is because your muscle tightens up and will not relax. These spasms usually occur as a reflex - meaning that you cannot control the contraction of the muscles. When any part of the spine is injured, including: a disc, ligaments, bones, or muscles, the muscles automatically go into spasm to reduce the motion around the area. This protective mechanism is designed to protect the injured area.
When muscles are in spasm they produce too much of the chemical, lactic acid. Lactic acid is a waste product produced by the chemical reaction inside muscle cells that must occur to allow the muscle to contract. If the muscle cell cannot relax, too much lactic acid builds up inside the muscles. The buildup of lactic acid causes a painful burning sensation.
The main reason that lactic acid builds up inside the muscle cells is that when the muscles contract, the small blood vessels traveling through the muscles are pinched off (just like a tube pinched between your thumb and finger). When the muscle relaxes, the lactic acid is eventually washed away by fresh blood flowing into the muscle as the blood vessels open up.
Spinal Segment
Back specialists sometimes look at a spinal segment to understand and explain how the whole spine works. A spinal segment is made up of two vertebrae attached together by ligaments, with a soft disc separating them. The facet joints fit between the two vertebrae, allowing for movement, and the neural foramen between the vertebrae allow space for the nerve roots to travel freely from the spinal cord to the body.
The spinal segment allows us to focus on the repeating parts of the spinal column to better understand what can go wrong with the various parts of the spine. Sometimes problems in the spine involve only one spinal segment, while other times the problems involve multiple segments.
Each spinal segment is like a well-tuned part of a machine. All of the parts should work together to allow weight bearing, movement, and support. When all the parts are functioning properly, all spinal segments join to make up a remarkably strong structure called the spinal column. When one segment deteriorates to the point of instability, it can lead to problems at that segment causing pain and other difficulties.
Now that you know the parts of the spine, let's look at the spine itself, which has three main segments - the lumbar, thoracic, and cervical spines.
Lumbar Spine
The lowest part of the spine is called the lumbar spine. This area has five vertebrae. However, sometimes people are born with a sixth vertebra in the lumbar region. The base of your spine (sacrum) is a fusion of many bones, and when one of them forms as a vertebra rather than part of the sacrum, it is called a transitional (or sixth) vertebra. This occurrence is not dangerous and does not appear to have any serious side effects.
The lumbar spine's shape has what is called a lordotic curve. The lordotic shape is like a backwards "C". If you think of the spine as having an "S"-like shape, the lumbar region would be the bottom of the "S". The vertebrae in the lumbar spine area are the largest of the entire spine, so the lumbar spinal canal is larger than in the cervical or thoracic parts of the spine. Because of its size, the lumbar spine has more space for the nerves to move about.
Low back pain is a very common complaint for a simple reason. Since the lumbar spine is connected to your pelvis, this is where most of your weight bearing and body movement takes place. Typically, this is where people tend to place too much pressure, such as: lifting up a heavy box, twisting to move a heavy load, or carrying a heavy object. Such repetitive injuries can lead to damage to the parts of the lumbar spine.
Thoracic Spine
The thoracic spine is made up of the middle 12 vertebra of the spine. These vertebrae connect to your ribs and form part of the back wall of the thorax (the ribcage area between the neck and the diaphragm). This part of the spine has very narrow, thin intervertebral discs, so there is much less movement allowed between vertebrae than in the lumbar or cervical parts of the spine. It also has less space in the spinal canal for the nerves. The thoracic spine's curve is called kyphotic because of its shape, which is a regular "C"-shaped curve with the opening of the "C" in the front.
Cervical Spine
The cervical spine is made up of the first seven vertebrae in the spine. It starts just below the skull and ends just above the thoracic spine. The cervical spine has a lordotic curve (a backward "C"-shape) - just like the lumbar spine. The cervical spine is much more mobile than both of the other spinal regions - think about all the directions and angles you can turn your neck.
Unlike the rest of the spine, there are special openings in each vertebra in the cervical spine for the arteries (blood vessels that carry blood away from the heart), as well as the spinal canal that carries the spinal cord. The arteries that run through these openings bring blood to the brain.
Two vertebrae in the cervical spine, the atlas and the axis, differ from the other vertebrae because they are designed specifically for rotation. These two vertebrae are what allow your neck to rotate in so many directions, including looking to the side.
The atlas is the first cervical vertebra - the one that sits between the skull and the rest of spine. The atlas does not have a vertebral body, but does have a thick forward (anterior) arch and a thin back (posterior) arch, with two prominent sideways masses.
The atlas sits on top of the second cervical vertebra - the axis. The axis has a bony knob called the odontoid process that sticks up through the hole in the atlas. It is this special arrangement that allows the head to turn from side to side as far as it can. Special ligaments between these two vertebrae allow a great deal of rotation to occur between the two bones.
Though the cervical spine is very flexible, it is also very much at risk for injury from strong, sudden movements, such as whiplash-type injuries. This high risk of harm is due to the limited muscle support that exists in the cervical area, and because this part of the spine has to support the weight of the head. This is a lot of weight for a small, thin set of bones and soft tissues to bear. Therefore, sudden, strong head movement can cause damage.
Pathological Concepts of the Spine
Back pain can be caused by a number of spinal conditions, and below are descriptions of various causes of discomfort:
Mechanical versus Compressive pain
Sometimes it is useful for back specialists to understand back problems by dividing the problems into different categories. One way to look at back pain is to divide problems into two large categories -- mechanical back pain and compressive back pain.
Mechanical pain is often called back strain because is linked with the movement, or "the mechanics" of the spine. This type of pain occurs when injury to the spine's discs, facet joints, ligaments, or muscles results in inflammation. It is called mechanical pain because it relates to the mechanics of your spine. The more you use the back, the more it hurts. This pain can be caused by many conditions in the spine. These conditions include: fractures of the vertebra, muscle strains in the paraspinal muscles, ligament injures in the spine, and wear and tear of the spine's joints and discs.
Compressive pain is a result of pressure or irritation on the spinal cord, or nerves that leave the spine. For example, if an intervertebral disc herniates (usually called a ruptured disc) and pushes into the spinal canal, it can cause problems with the nerve. Usually this pressure or irritation causes pain, numbness, and muscle weakness where the nerve travels.
Each part of the spine can cause pain. It can be helpful to understand which part of the spine is causing your back pain and whether the pain is from a compressive or mechanical type problem.
Arthritis Pain
The term arthritis means inflammation of the joints. Arthritis of the spine usually refers to a condition where there is inflammation of the facet joints between the vertebrae. The pain that results from arthritis is usually the mechanical type of back pain. If bone spurs develop due to the arthritis and begin rubbing on the spinal nerves, there can also be compressive type pain produced as well. There are two types of arthritis: systemic inflammatory arthritis, and wear-and-tear arthritis. A systemic type of arthritis is actually a disease process that affects all the joints of the body - such as rheumatoid arthritis. Many arthritis type diseases affect the connective tissues of the body. All of these diseases cause inflammation of the joint tissues and destruction of the joints. The joints of the spine may be involved in systemic types of arthritis because the facet joints are made up of the same tissues as any other joint. Therefore, diseases that attack joint tissues also attack the facet joints.
Wear-and-tear arthritis, or osteoarthritis, can result from many things. It can come from a single injury that damages the joint. It can also result from a lifetime of overuse of different joints that damage the joint a little bit at a time. Doctors are now beginning to realize that osteoarthritis also runs in families. Something about the genetic makeup of different individuals makes them more prone to develop osteoarthritis of various joints.
Osteoarthritis is caused by a permanent breakdown of the articular cartilage inside the affected joint. Articular cartilage is the material inside the joint that cushions the bones of the joints from impact and allows smooth, gliding motions. Because damaged cartilage cannot repair itself, it begins to fray, making it less flexible and more prone to injury. Over time, the cartilage can wear away completely, causing the bony surfaces of the joint to rub directly against each other. Eventually the joint becomes worn away and bone spurs develop around the joint.
Facet Joint Syndrome
Sometimes the facet joints are the main cause of back pain. In many cases, the facet joints are at least part of what is causing your back pain. When your doctor thinks the facet joints are a major source of your pain, he may use the term "facet joint syndrome". Facet joint degeneration, or osteoarthritis, can be caused by a combination of aging, pressure overload of the facet joints, and injury.
Pressure overload on the facet joints is probably caused by degeneration of the intervertebral disc. As the discs degenerate, they wear down and begin to collapse. This narrows the space between each vertebra. This narrowing of the space between each vertebra affects the way the facet joints line up. When this occurs, it places too much pressure on the articular cartilage surface of the facet joint. The excessive pressure leads to damage of the articular surface and eventually the cartilage begins to wear away.
When facet joint arthritis gets bad enough, the cartilage and fluid that lubricate the facet joints are eventually destroyed as well, leaving bone rubbing on bone. Bone spurs begin to form around the facet joints. When bone spurs develop, they can take up space in the foramen (the opening between vertebrae where nerve roots exit the spine) and press into nerve roots. As the bone spurs begin to grow larger, they can eventually extend into the spinal canal itself. This leads to narrowing of the spinal canal (spinal stenosis).
Pinched Nerve (Radiculopathy)
Radiculopathy is the medical term used to describe a "pinched nerve" in the spine. A radiculopathy occurs when a nerve is irritated by something that is either rubbing on the nerve or pressing on the nerve. In some cases, such as a herniated (or ruptured) disc, there may also be a chemical reaction irritating the nerve. Chemicals released from the inside of the disc seem to irritate nerve tissue, causing pain and inflammation of the nerve.
Abnormal pressure or irritation on a particular nerve causes several problems. First, there is numbness in the area where the nerve usually provides sensation, or feeling. For example, if the nerve usually ends in the side of the foot and supplies sensation to that area, it will have decreased feeling, and often pain.
The key to understanding a radiculopathy is understanding that your brain cannot tell where the problem really is. While the irritation or pressure on the nerve may be in your back, your brain thinks the pain is coming from your foot. In addition, the muscles that the nerve usually controls will not work right. You will usually have weakness in the muscles, and the reflexes controlled by the muscles will not work. This is why doctors always check reflexes. The body has a pretty standard wiring diagram. By determining which reflexes are not working, the doctor can usually tell which nerve is involved with the problem.
Things that can cause a radiculopathy include: herniated discs, bone spurs, tumors that are growing into the nerves, and fractures that put pressure on the nerves.
Sciatica
The term sciatica refers to a certain type of radiculopathy that occurs in the leg. It is called sciatica because it describes the radiculopathy that occurs when one or more of the nerves that make up the large sciatic nerve are irritated or pinched. Therefore, sciatica is not any different than a pinched nerve anywhere else in the spine. It simply has its own name because it is fairly common. It also occurs in the lumbar spine, the most common site of spinal nerve irritation.
Sciatica is used to describe the pain that travels from the sciatic nerve in the lumbar region into your buttocks, back of the thighs, and sometimes calf and foot. The pain is typically caused by irritation of the nerve roots that join outside the spine to make up the sciatic nerve. Conditions that can cause sciatica are: herniated discs, bone spurs, cancerous tumors that are growing into the nerves, and fractures that put pressure on the nerves.
Spinal Cord Pressure
We have seen how individual nerve roots are affected by pressure and irritation -- but what about the spinal cord itself? Pressure on the spinal cord typically results from a condition called stenosis. Stenosis means narrowing of an opening or tube - in this case the spinal canal.
Spinal Stenosis
Spinal stenosis is a term commonly used to describe a narrowing of a portion of the spinal canal. Stenosis can occur in all areas of the spine, but it is most common in the cervical and lumbar spine. There can often be narrowing of most of the lumbar spinal canal and of several segments of the cervical spine. Each behaves somewhat differently.
Although there is some space between the spinal cord and the edges of the spinal canal, this space can be reduced by many conditions. Bone and tough ligaments surround the spinal canal. This tube cannot expand if the spinal cord or nerves require more space. If anything begins to narrow the spinal canal, the risk of irritation and injury of the spinal cord or nerves increases. Some conditions that can lead to narrowing of the spinal canal include: infection, tumors, trauma, herniated disc, arthritis, thickening of ligaments, growth of bone spurs, and disc degeneration.
Spinal stenosis usually occurs in older people after years of wear and tear or degeneration of the spine. This wear and tear results in changes in the structures around the spinal canal, such as thickening of the large ligaments that connect the vertebra together, bone spurs around the facet joints and disc space, and bulging of the discs themselves. All of these changes push into the spinal canal, making the tube of the spinal canal smaller. Eventually, there is not enough space in the spinal canal for the nerve to comfortably fit without causing too much pressure. Stenosis can also develop because of injuries, infections, or tumors. Some people even have a narrow spinal canal from birth, and this abnormality leads to symptoms of stenosis.
The narrowing of the spinal canal can lead to irritation of the nerves of the spine. This can cause pain and problems with the nerves not working right. The lack of space can also cause the supply of blood and oxygen to the spinal cord to be reduced. When the spine needs more blood flow during increased activity, the blood vessels may not be able to swell to get more blood to the spine. This can lead to numbness and pain in the affected nerves. The nerves also lose some of their mobility when the space available to them is reduced. This leads to irritation and inflammation of the nerves.
Other symptoms of spinal stenosis include: a sensation of heaviness, weakness, and pain when walking or standing for a long period. With rest, these symptoms often disappear. These symptoms occur because the nerve roots are being tampered with, upsetting the normal signals that travel from the brain to the body. Irritation of the nerves in the spinal canal is worse when with standing or walking because of the mechanical compression and stretching of the nerves.
Segmental Spinal Stenosis
Segmental spinal stenosis is a narrowing of the spinal canal in a segmented, or specific, area. Sometimes the stenosis only occurs in a small area of the spine, such as an area where there is a combination of bone spurs from the facet joints in the back of the spinal canal and a bulging disc in the front of the spinal canal. This results in narrowing of that one area of the spine.
Segmental stenosis can occur in both older and younger people. The symptoms of segmental spinal stenosis are similar to other conditions of the spine. Segmental spinal stenosis can affect the nerve roots that leave the spine at the area where the segmental stenosis occurs. These nerves can become irritated, causing pain, numbness, and weakness in the area the nerve travels. There can also be pressure on the rest of the spinal nerves that must travel through the narrowed area of the spinal canal.
Discogenic pain
Discogenic pain is a term back specialists use when referring to pain caused by a damaged intervertebral disc. A degenerating disc may cause pain of the mechanical type. As the disc begins to degenerate, there is some evidence that the disc itself becomes painful. Movements that place stress on the disc can result in back pain that appears to come from the disc. This is similar to any other body part that is injured, such as a broken bone, or even a cut in the skin. When these types of injuries are held still, there is no pain. However, if you move a broken bone, or the skin around a cut, it causes pain.
Discogenic pain usually causes pain felt in the lower back. It may also feel like the pain is coming from your buttock areas and even down into the upper thighs. The experience of feeling pain in an area away from the real spot causing the pain is common in many areas of the body, not just the spine. Examples include: a person who has gallstones may feel the pain in their shoulder; or a person experiencing a heart attack may feel pain in the left arm. This is called radiation of the pain. It is very common for pain produced by spine problems, such as disc problems, to be felt in different areas of the body, including the back itself.
Bulging Disc
Bulging discs are fairly common in both young adults and older people. They are not cause for panic. In fact, abnormalities that show up on MRIs, such as bulging or protruding discs, are seen at high rates in patients both with and without back pain. Most likely, some discs begin to bulge as a part of the aging process, and the degeneration process of the intervertebral disc. A bulging disc is not necessarily a sign that anything serious is happening to your spine.
A bulging disc becomes important when it bulges enough to cause narrowing of the spinal canal. If there are bone spurs present on the facet joints behind the bulging disc, the combination may cause narrowing of the spinal canal in that area. This is sometimes referred to as segmental spinal stenosis.
Herniated Disc
A herniated disc occurs when the intervertebral disc's outer fibers (the annulus) are damaged and the soft inner material of the nucleus pulposus ruptures out of its normal space. If the annulus tears near the spinal canal, the nucleus pulposus material can push into the spinal canal. This can cause too much pressure on the spinal cord and nerve roots. There is also some evidence that the nucleus pulposus material causes a chemical irritation of the nerve roots. Both the pressure on the nerve root and the chemical irritation can lead to problems with how the nerve root works. The combination of the two can cause pain, weakness, and/or numbness in the area of the body to which the nerve travels. For this reason, a herniated disc usually causes pain of the compressive type. Sometimes a herniated disc is referred to as "slipped disc", though the disc does not actually slip.
Herniated discs are common in the lumbar spine because of all the pressure it supports. A herniated lumbar disc often produces sciatica. This is a condition where the lower back pain and numbness radiates down the back of the leg, side of the calf, and possibly into the side of the foot. You may not necessarily have much back pain. The exact area where you will feel numbness depends on the nerve root that is affected; the numbness could be in the inner ankle, big toe, heel, outer ankle, outer leg, or a combination of them. Your doctor can use this information to get an idea which nerve is affected.
Pressure on the nerve root can cause the parts of the nerve that control the muscles not to work properly. This can result in weakness of some muscles and may change the reflexes in certain areas. Again, your doctor can use this information to try to determine which nerve is involved.
The same is true for the neck. A problem stemming from the neck may result in pain that is perceived in the arm or hand. However, a herniated disc is much less common in the thoracic spine. This is likely because the discs are much thinner and there is less material in the nucleus pulposus to rupture into the spinal canal. HOWEVER, if a herniated disc does occur in the thoracic spine, it can be much more serious than in the lumbar spine. The thoracic spine has very little extra room in the spinal canal. In addition, a herniated disc in the thoracic spine puts pressure on the spinal cord - not just a few nerve roots. Too much pressure on the spinal cord from a herniated thoracic disc can lead to total paralysis from the waist down.
Just because a disc has herniated does not necessarily mean that you will need to undergo surgery. In most cases, a herniated disc can be treated without surgery. The treatment of a herniated disc depends on the symptoms. It also depends on whether the symptoms are getting steadily worse -- or whether they are getting better. If the symptoms are getting steadily worse, your doctor may be more likely to suggest surgery. If the symptoms are getting better, your doctor may suggest watching and waiting to see if the symptoms go away. In many cases, the initial problems due to a herniated disc completely resolve over several weeks to months.
In rare cases, a herniated disc in the lumbar spine area can be so large that it fills the entire spinal canal in the area where it ruptures. When the spinal canal fills with disc material, it may place a great amount of pressure on the nerves. If this occurs in the lower spine, it can lead to a condition called "cauda equina syndrome". This problem can lead to permanent paralysis of the muscles that control your bowels and bladder. If you lose control over your bladder or bowels, you should contact your health care provider immediately. These symptoms require immediate medical attention.
Copyright © 2003 DePuy Acromed.
